An Innovation in Provider Training Increases Access to Care for Sickle Cell Disease Patients
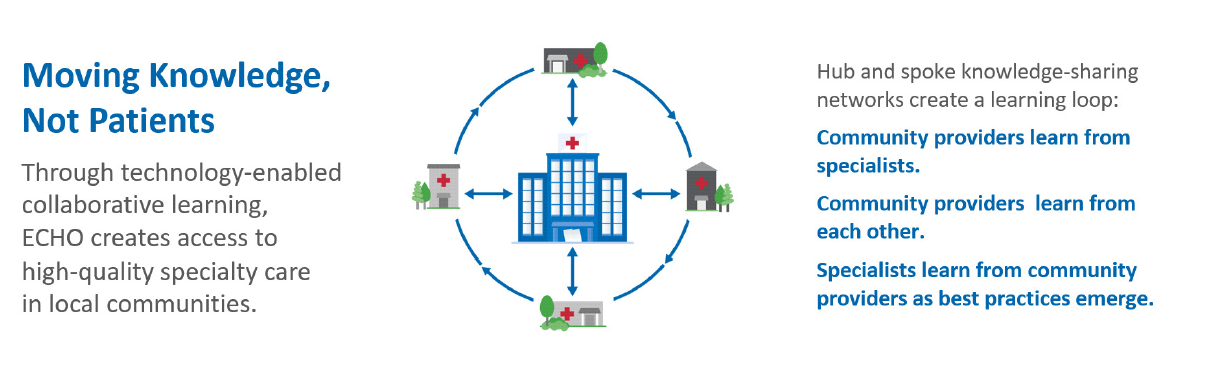
Project ECHO® (Extension for Community Healthcare Outcomes), developed by and disseminated through the University of New Mexico Health Sciences Center, uses telementoring to train and ultimately increase the number of clinicians knowledgeable about specialty disease care, like SCD, so that more patients can receive expert care that is timely and convenient. By developing hub-and-spoke knowledge-sharing networks, where an expert team (the hub) provides virtual learning sessions to community providers (the spokes), Project ECHO creates a continuous learning loop between specialists and community providers.
In the past five years, Project ECHO telementoring hubs for SCD have spread across the U.S., fostering a rapidly growing national network for SCD training and knowledge-sharing. While SCD ECHO hubs are regionally based, their virtual learning teleECHO™ programs are open to community providers across the country, and in some cases, attended by individuals across the world. Each hub is managed by a designated regional coordinating center (RCC), who are grantees of the federal Sickle Cell Disease Treatment Demonstration Regional Collaborative Program (SCDTDRCP), and both funded and managed by the US Health Resources and Services Administration (HRSA).
As the national coordinating center for the demonstration program, NICHQ provides technical support to the five regional coordinating centers, helping them align efforts and ensure uniform data collection and analysis.
Interested in learning more about telementoring’s potential to improve access to SCD care? Below, team leads from three different regions of the U.S. expand on the benefits of this innovative approach to SCD provider education.
Making miles matter less
While SCD patients live across the country, SCD specialists often reside in large urban settings near research hospitals and specialty care centers. As a result, a patient living in rural Indiana, for example, may need to travel more than a hundred miles to be seen by an expert in Indianapolis.
Increasing knowledge among community providers—including adult primary care providers, pediatricians, nurses, advanced practice providers, and community hospital providers—can help more patients access evidence-based treatments and high-quality care. But many community providers have little experience treating a rare disease like SCD, and the learning requirements are constantly shifting as new treatments, best-practices, and protocols emerge.
“It’s a massive struggle to connect primary care providers who are dispersed across the country to the information they need or the experts who can support them, who are often far away,” confirms Michael Rowland, the Telehealth Coordinator for Pacific Sickle Cell Regional Collaborative (PSCRC). “Telementoring is changing that.”
Telehealth technology, such as video conference calls, helps expert interdisciplinary specialists connect with community providers through virtual learning sessions. In a typical learning session, specialists share insights, case presentations, and didactic educational sessions on the many different topics that affect patient care.
Flexible, cost-effective and targeted education
“Because ECHO learning sessions are free, short term and flexible to attend, we can cost-effectively offer training to providers who may not have had funding or reimbursable billing hours to devote to a disease that affects so few of their patients,” says NICHQ Project Manager Barbara Lambiaso. “This is one of the reasons telementoring programs are critical for SCD care—they create, accessible, sustainable provider education, which increases access… for SCD patients across the country.”
Like funding, time is an easily depleted resource for providers. That’s why having teleECHO sessions focused on different topics, operating out of different regions, and happening at different times is essential, says Northeast RCC lead Roslyn Stewart, MD, MBA, MS. When providers have more options, they can prioritize relevant learning sessions that address their specific needs.
“ECHO without limits—that’s the goal,” says Stewart. “So, if you live in Boston but you’re interested in a topic from a Midwest ECHO session, or the time just works better for you, then you can attend that learning session. You can choose to attend what makes sense for you.”
Are you a provider interested in learning about SCD care through Project ECHO? Click here to find out about the upcoming telementoring sessions.
Concerted advertising helps give all providers an opportunity to benefit from the different offerings, explains Lisa Shook, MA, MCHES, who leads the Midwest RCC. Offering Maintenance of Certification credits, sharing upcoming learning sessions in regional and national newsletters, and identifying champions who can spread the word to their networks all help raise awareness.
And while advertising is an ongoing challenge, the spread of the work is evident, says Stewart: “In four years, the Northeast ECHO learning sessions have reached over 1,300 individuals in 22 states and three countries.”
Creating a community of SCD stakeholders
Along with connecting community providers to specialists, telementoring also encourages collaboration and knowledge-sharing between community providers.
“Even though the learning is virtual, you feel this sense of family,” says Stewart. “Whether we’re working through a difficult case or talking about a family and what they’ve gone through, it’s comforting to problem solve with other providers—to know that we’re all working together to improve outcomes for patients living with sickle cell disease.”
As a platform for collaboration, SCD ECHO programs can also help address one of the biggest challenges facing SCD patients: the rise in morbidity and mortality rates that occurs when patients transition from pediatric to adult care.
This increase is in part linked to a lack of coordination and communication between providers during this important time, says Rowland. “Having providers from all across the lifespan join a virtual learning session helps break down barriers between the two groups.”
And it’s not just healthcare providers who benefit from this community, adds Shook. Community health workers, pharmacists, hospital administrators, professionals from community-based organizations, state health departments, and insurance companies can all tap into relevant teleECHO sessions, building knowledge among the many different groups of people needed to provide SCD patients with comprehensive care and support.
Over the next four years, each RCC will continue to develop their SCD ECHO programs, building a robust national network that can support SCD patients across the country, from infancy to adulthood. Stay informed about their successes and lessons-learned by signing up for NICHQ News.
