Gender-affirming healthcare consistently shown to reduce health disparities for youth
March 31 is Transgender Day of Visibility and Action, closing a week of awareness celebrating strides in visibility, advocacy, and community. Unfortunately, this year has also brought a concerning surge of anti-trans and anti-LGBTQI legislation across the United States, even as new research is published on the low regret rates from gender-affirming care.
As public health professionals often on the front lines advocating for children’s health, we encourage you to continue your advocacy for evidence-based standards of care created by respected organizations comprised of physicians, endocrinologists, and mental health experts. We all can contribute to an information-based environment where decisions are made based on health outcomes, not hate or fear.
How many youth are transgender?
According to the AAP, questions related to gender identity are rarely asked in population-based surveys, which makes it difficult to assess the size and characteristics of the population who is transgender or gender-diverse. According to the Williams Institute at UCLA School of Law, recent data from both the YRBSS and the CDC’s Behavior Risk Factor Surveillance System (BRFSS) create an opportunity to update prior populations of how many youth ages 13-17 identify as transgender in the U.S. Since 2017, only 15 states have elected to include optional questions on gender identity in the Youth Risk Behavior Surveillance System (YRBSS) Survey of the Centers for Disease Control and Prevention. It is potentially still an underestimate given the stigma regarding those who openly identify as transgender and the difficulty in defining “transgender” in a way that is inclusive of all gender-diverse identities.
Using data from the 2017 and 2019 YRBSS and the 2017-2020 BRFSS, the Williams Institute found that among youth ages 13 to 17 in the U.S., 1.4% (about 300,000 youth) identify as transgender. This is about double previous estimates. Research also showed that transgender individuals are younger on average than the U.S. population. They found that youth ages 13 to 17 are significantly more likely to identify as transgender (1.4%) than adults ages 65 or older (0.3%).
A February report from the American Medical Association confirmed that lack of access to puberty blockers or hormone therapy was strongly correlated with poor mental health and suicidal ideation among trans youth. Conversely, and powerfully, research released on March 29 shows that transgender and nonbinary young people who came out about their gender identity and had high family support reported lower rates of considering and attempting suicide in the past year.
The very same week in March, one state’s Legislature overrode its Governor’s veto of a gender-affirming care ban bill called one of the “most extreme” pieces of anti-LGBTQ legislation in the country by the Human Rights Campaign, the ACLU, and The Trevor Project, an LGBTQI+ suicide prevention support service. In addition to banning puberty-blockers, hormones, and surgeries for kids under 18, the bill would also ban lessons on gender identity and sexual orientation in public schools, prevent trans students in public schools from using the bathroom that corresponds with their gender identity, and stop school districts from requiring teacher’s use a student’s pronouns if they don’t align with their sex assigned at birth.
Although data exist that show nearly 1 in 5 trans or nonbinary youth have attempted suicide due to the impact of discrimination and bias (and more concerningly, 1 in every 4 Black trans or nonbinary youth), copies of this bill are being enacted across the U.S. In total, more than 425 pieces of legislation in 2023 have targeted youth, a substantial increase from last year, when more than 335 pieces of legislation aimed at controlling the existence of gender-diverse children and adolescents were introduced in state legislatures. A poll from The Trevor Project showed that 85% of transgender and nonbinary youth and 66% of all LGBTQI+ youth said that recent debates around anti-trans bills have negatively impacted their mental health. Children of all identities thrive when they feel heard, accepted, supported – the opposite of what this legislation does.
Health Disparities for LGBTQI+ Youth
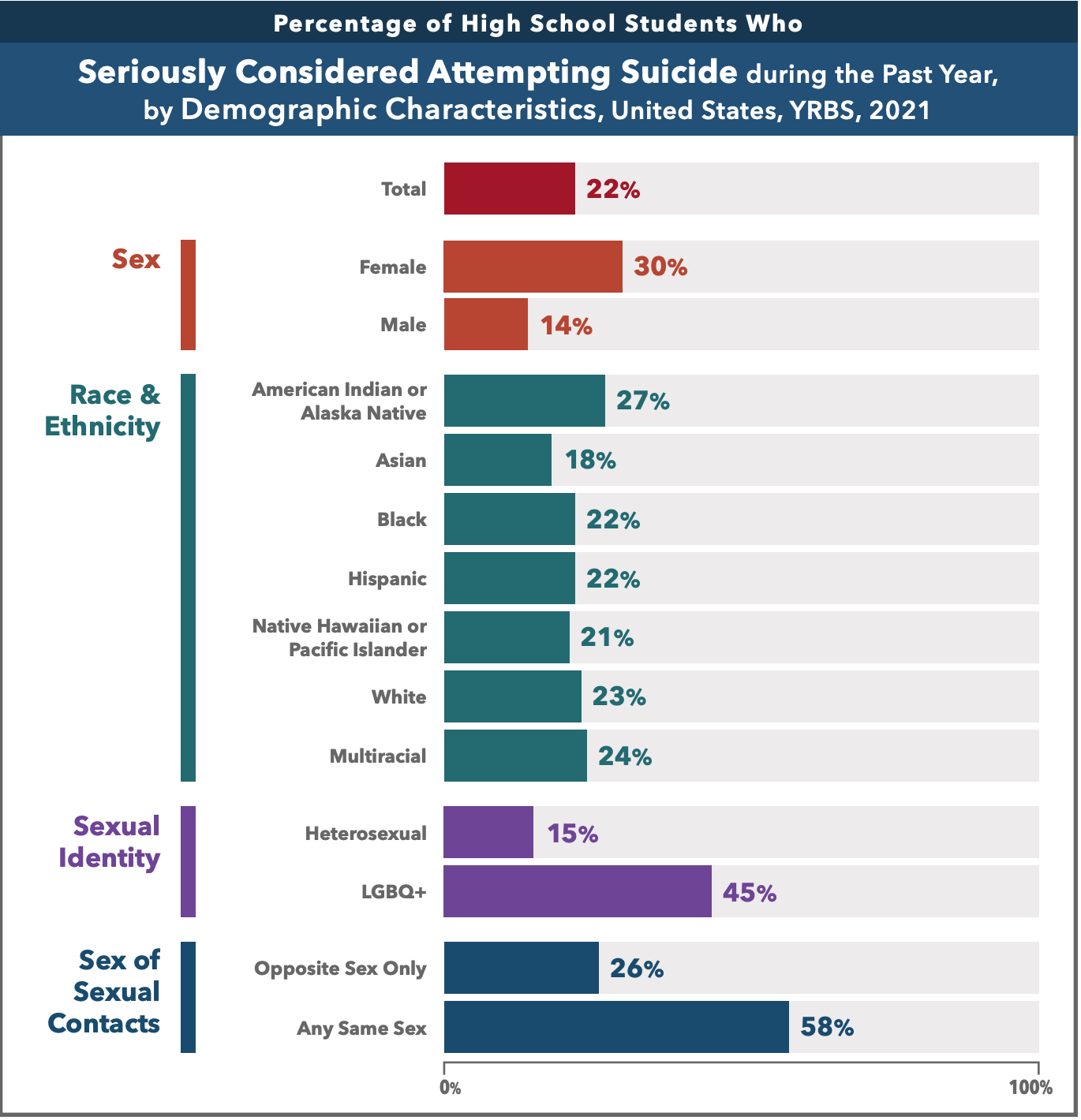
These factors, combined with a lack of support from family and bullying from peers, are why we are losing more LGBTQI+ youth to suicide than ever before, and anti-LGBTQI+ violence is on the rise. In the CDC’s Youth Risk Behavior Surveillance (YRBS) Survey Summary Trends Report 2011-2021, a survey fielded to U.S. students, it was noted that sexual minority youth (SMY) are at increased risk for negative health and life outcomes – not from being LBGTQI+ but as a result of bias, stigma, and discrimination. CDC research has found that compared to their peers, SMY have a higher risk of suicide, depression, substance use disorder, and poor academic performance. In 2021, SMY youth were three times as likely to have “seriously considered attempting suicide” during the past year compared to their straight peers (Fig. 1).
The YRBS formerly included trend information also segmented by sexual identity, but the most recent trends report omitted these due to updates in language to make options more inclusive. Disparities viewed through the SMY lens are higher than for any other demographic category measured, so monitoring year-to-year trends is important. Future iterations of the YRBS will share more on the experience of transgender students, but all existing research points to larger disparities for this group.
As physicians, public health professionals, and other healthcare providers, we have an obligation to support these youth with unique healthcare needs who are at higher risk for negative health outcomes from discrimination, bullying, physical assault, and suicide. Join us by engaging in meaningful dialogue about best practices for gender-diverse kids to improve their quality of life, reduce mental health disparities, and through an intersectional lens, help the most historically marginalized kids achieve their optimal health. Because they experience marginalization on multiple levels, BIPOC youth who are also transgender or nonbinary face the largest health disparities of all – and we should center them in our shared conversations and approaches.
